Sidelined by cancer during COVID, Holy Spirit medical assistant gets back to her patients at vaccine site
Welcome to your life after COVID-19. Meet your guide, Renee Still.
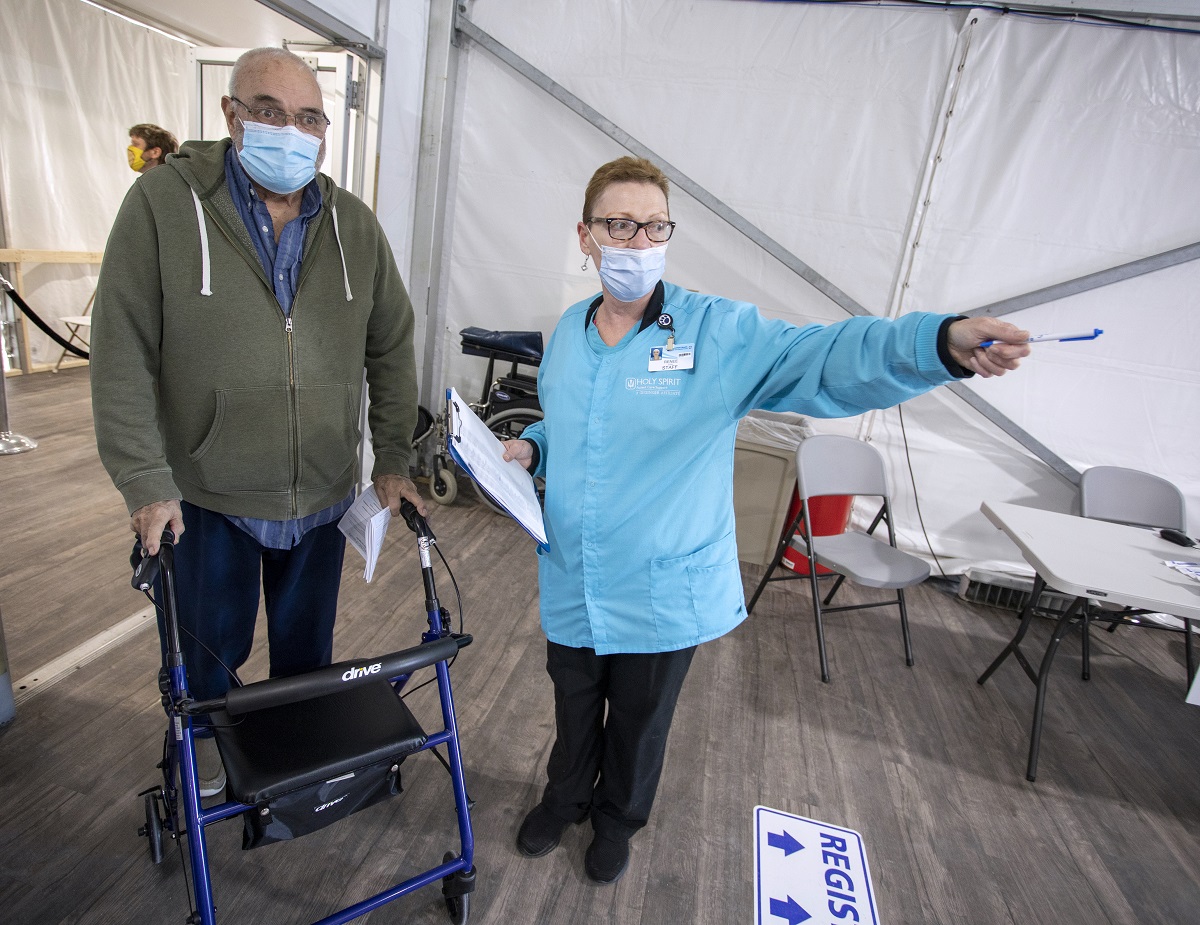
“Hi there!” she says with a voice that simultaneously hits 10s on gauges for volume and warmth. You meet her when you first enter the dedicated vaccination site at Penn State Health Holy Spirit Medical Center. Still is the last stop between you and the vaccine everyone hopes will send the year-old pandemic into history’s ash bin. Once you’re inside the tent, Still tells you where to sit to get your shot.
Her eyes are smiling above her surgical mask and beneath her close-clipped mop of rust-colored hair. “It used to be long curls,” she’ll tell you, but don’t look at the Penn State Health ID she’s wearing for a glimpse of her old hair.

Renee Still’s ID badge shows a photo from November, when she going through chemotherapy treatments during her third battle with cancer.
In that photo, Still stares defiantly into the camera under a skullcap to hide one of the side effects of her chemotherapy.
“Cancer is a pain in the keister,” Still said. It’s her third wrestling match with it. The first was 18 years ago. Her latest positive test came two years ago. She just finished her fifth chemotherapy treatment at Hershey Medical Center and is soon due for a test to determine how much good it did.
Still has worked for Holy Spirit for the past 27 years as a medical assistant. Her most recent gig in the Medical Center’s presurgery clinic was to help prepare patients for dates with scalpels. She took vitals, blood samples and EKG scans. Still has all the prerequisites for the job. She loves people, particularly meeting new ones and sharing with them the laughs which for her come easily.
When the pandemic arrived, Still’s doctors told her she couldn’t touch COVID-19 with a 10-foot pole because of the toll cancer and treatment had taken on her immune system. So, to protect her, the Medical Center moved her to the basement of the Camp Hill facility, miles from the worst of the coronavirus, where she worked screening contractors entering the building for COVID-like symptoms.
The blow was twofold. Not only couldn’t Still visit with the patients she loved, she was also sidelined during the biggest health crisis of the past hundred years.
But Still rolled with it. “I learned a lot. I met fascinating people,” she says of her time in the basement. “For the first time, I really learned how the hospital operates.”
By the time the vaccine arrived and Holy Spirit announced plans to open the site in a tent adjacent to the hospital, Still had shifted back to the presurgery clinic, but the department had become largely inactive during the surge of the late fall and winter months.
Still was anxious to get back to work among the patients she loved. She asked the nurse manager if there was something – anything ― she could do. The nurse manager landed her a spot in the vaccine tent. Her doctors at Hershey Medical Center told her it was OK, so on Feb. 22, when the dedicated vaccination site officially opened, Still arrived to help ferry patients to the right destinations.
“All righty, my dear, come on back,” she sings to an elderly woman whose turn has arrived. “We’re going to get you to No. 2.”
The warmth is welcome. Michele Moppin, a guard with Allied Security, helps greet the patients arriving in cars and lets them know the drill. The people wait inside their cars for roughly 15 minutes before someone tells them to go to another tent for screening.
“Some of them are scared,” Moppin says. “Some of them are emotional.”
Many have questions. How will the vaccine react with this other medicine I’m taking? What kinds of side effects will I have?
Dr. Andrew Walker of Holy Spirit’s Department of Internal Medicine is stationed just inside the tent to dispense answers. He’s one of many intangibles the site’s planners have compiled – from small, battery-powered timers that let patients know they’re free to leave after receiving the shot to changing ways to dispose of needles. Some intangibles, like Walker, were part of the initial design. Others, like the sandwich boards in front of each station telling patients what step they’re on and where to go next, came about through later fine-tuning.
Among the intangibles is Still. From her, patients get a friendly voice during a stressful time. And Still gets back to her old friends she hasn’t yet met.
“It’s fabulous,” she says, with a smile you can see beneath her mask. “I love it.”
If you're having trouble accessing this content, or would like it in another format, please email Penn State Health Marketing & Communications.
