‘I wish I hadn’t waited so long.’ Berks County woman thrives after weight loss surgery at Penn State Health Lancaster Medical Center.

Daily living had become difficult for Trina Love.
At her peak weight of just over 300 pounds, performing simple chores was hard, and the 50-year-old Berks County woman experienced frequent pain in her feet and ankles.
“I was having trouble breathing,” recalled Love, who is 5-foot-3. “I couldn’t even walk up the stairs.”
Ultimately, Love chose the surgical weight loss program at Penn State Health Lancaster Medical Center in East Hempfield Township, a decision she said dramatically improved her life.
An emotional eater
Love’s struggles with her weight intensified after her son was diagnosed with a brain tumor at age 5. Her daughter was born shortly after her son’s diagnosis, making life even more complicated.
“I couldn’t shed the weight after my daughter was born, and it was especially hard with my son battling a brain tumor,” she said. “I’m an emotional eater, and that’s how I coped.”
Knowing she had to make some changes, Love started researching bariatric surgery. Even though she had hired a physical trainer and lost 65 pounds in the previous nine months, it wasn’t enough to resolve her persistently high blood pressure and other health issues.
“I tried to educate myself on all the pros and cons of surgical weight loss before making any decisions,” she said. “After a lot of thought, I decided to get it.”

Dr. Allison Barrett meets with Love during her one-year follow-up appointment after weight loss surgery.
Personalized approach
Love recalled her first visit to Penn State Health Medical Group – Noll Drive, where she met Dr. Allison Barrett, director of bariatric surgery at Lancaster Medical Center, who would perform Love’s surgery.
“Right away, I felt like Dr. Barrett was someone who had my best interests at heart,” Love said.
Other members of the surgical weight loss team were equally supportive.
“They kept me motivated by encouraging me to continue exercising and watching what I was eating as I prepared for surgery,” Love recalled. “They took a very personalized approach to my care.”
After meeting several times over a period of months with Barrett, as well as a nurse practitioner, dietician and a social worker who assessed her mental health, Love was cleared for the procedure. It takes approximately three to six months to prepare a patient for surgery.
Rapid recovery
Barrett, who with her surgical partner Dr. Parth Sharma performs approximately 75 gastric sleeve and gastric bypass procedures a year, conducted Love’s sleeve surgery in November 2022 using a da Vinci Surgical System. The minimally invasive, robotic surgery system makes smaller incisions, reducing pain and promoting a faster recovery.
Barrett credits typically short stays for bariatric surgery patients to the hospital’s “enhanced recovery after surgery” program.
To schedule an appointment to discuss weight loss surgery at Lancaster Medical Center, call 844-280-8209.
“We’ve seen excellent results from that post-surgery program,” she said. “The vast majority of our patients do extremely well after surgery.”
Patients are given liquids within a few hours of surgery, providing early access to calories and nutrition that help speed recovery. They normally stay on a liquid diet, including protein shakes, yogurt, pudding and thin soups, for about two weeks after surgery, then can start eating other foods.
The program reduces the amount of narcotic and opioid drugs patients get by substituting a nonsteroidal anti-inflammatory drug. Patients also receive a long-acting injected medication that numbs the abdominal wall for two to three days after surgery. Many patients report using only a few doses of a narcotic pain medication because they feel comfortable without it.
Minimal use of narcotics means patients are much more alert and able to be active after surgery. Patients are expected to get up and walk a couple of hours after their operations and are strongly encouraged to keep moving throughout their hospital stays and when they return home.
Walking helps with digestion and prevents blood clots. It also plays a crucial role in mental health during recovery. Doing this activity early on makes it possible for patients to get back to their normal lives more quickly.
Love followed a liquid diet for two weeks after surgery and said she was largely inactive for the first week, but suffered no serious effects.
“I had no nausea or problems with my fluid intake,” she noted. “I went back to work after two weeks.”
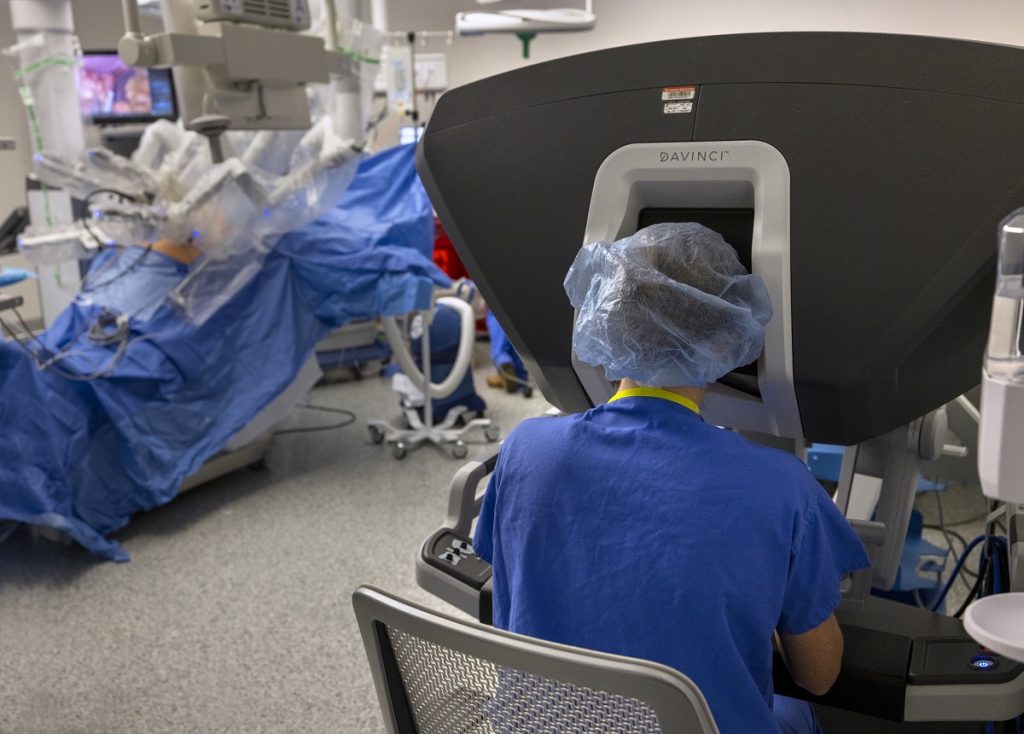
Dr. Allison Barrett uses a da Vinci Surgical System to conduct a sleeve gastrectomy procedure. The minimally invasive system uses smaller incisions, which reduces the risk of complications.
A tool, not a magic bullet
Taylor Ford, a nurse practitioner in the hospital’s bariactic surgery practice, said patients are encouraged to adopt healthy eating and exercise habits prior to surgery, as Love had, and should expect to maintain them indefinitely.
“Patients need to understand that surgery is a tool, not a magic solution,” she said. “They have to put in the work and stick to those good habits for the rest of their lives to be successful with their weight loss.”
Barrett agreed, saying obesity is a chronic disease and more than one treatment is required to address it. Patients who only need to lose a modest amount of weight may benefit from weight loss medications, but surgery remains the gold standard for those with more weight to lose or who cannot afford the medications, which can be cost-prohibitive.
Also, she noted, patients who stop using weight loss drugs due to cost or unpleasant side effects tend to regain the weight they lost because their appetites return, often with even higher hunger levels than previously.
“The decision on how to best lose weight requires an honest conversation between the doctor and the provider,” Barrett said. “Not every treatment is appropriate for every patient.”
One year later
One year after surgery, Love weighs 165 pounds, works out at a gym a couple of times a week and pays close attention to her diet. She’s reduced her body mass index from 44 to 28 and enjoys much improved mobility and less discomfort in her joints. Sticking to healthy habits can be challenging, she said, but it has made a huge difference in her life.
“Looking back, I wish I hadn’t waited so long to have surgery, but I think the timing turned out right because I was prepared physically and mentally for it, and I’ve been able to cope well,” she said. “It isn’t always easy, but I get to be here for my family, and it’s totally worth it.”
If you're having trouble accessing this content, or would like it in another format, please email Penn State Health Marketing & Communications.
