The Medical Minute: Tossing and turning? 5 ways to get a good night’s sleep

Few things are more frustrating than trying – and failing – to get a restful night’s sleep. March is Sleep Apnea Awareness Month, a good time to remember that sleep problems aren’t always caused by stress or busy schedules – sometimes they start in the body. Whether you struggle to fall asleep or wake up tired, chronic exhaustion shouldn’t go untreated. The good news? There are plenty of ways to help you get better sleep.
Dr. Matthew Floyd, a sleep medicine physician at Penn State Health Sleep Research and Treatment Center, says people should talk to a doctor if sleep issues are affecting their daytime life or family. Often, a bed partner is the first to notice the signs – unusual breathing or loud snoring during the night.
“If your sleep is negatively affecting your day-to-day functioning, you should come in and get evaluated,” Floyd says. ”Patients who have significant daytime sleepiness tend to have worse health outcomes.”
Sleep Apnea Explained
Abnormal breathing patterns often indicate sleep apnea, the most common condition Floyd treats. Patients stop breathing for short periods, depriving the brain of oxygen and triggering frequent wakeups or snoring. Sleep apnea comes in several types, but the most common is obstructive sleep apnea (OSA).
Dr. Neerav Goyal, division chief of Head and Neck Oncology and Surgery at Penn State Health College of Medicine, says OSA occurs when the airway gets blocked during sleep, often when the soft tissues in the throat relax and narrow the breathing passage. Sleeping on your back is a frequent cause.
For mild OSA, simple changes like wedge pillows that keep the sleeper on their side may be enough. Moderate cases can use an oral appliance, like a specially designed retainer that repositions the tongue or jaw to keep the airway open. Higher body weight and gastroesophageal reflux disease can worsen OSA, and many patients see immediate improvement from weight loss.
The most common treatment for OSA is a continuous positive airway pressure (CPAP) machine worn over the face while sleeping.
“A CPAP machine pushes air down your windpipe, making that tube bigger or stiffer, so the apnea doesn’t occur,” Goyal says. “But CPAP machines are cumbersome and can make some people claustrophobic. About 40% to 60% of patients prescribed a CPAP machine don’t use it regularly.”
Patients with severe OSA who can’t tolerate a CPAP machine can consider surgery. Goyal says that, historically, procedures have included removing the tonsils, removing the uvula – the small piece of tissue hanging in the back of the throat – or reducing the size of the back of the tongue.
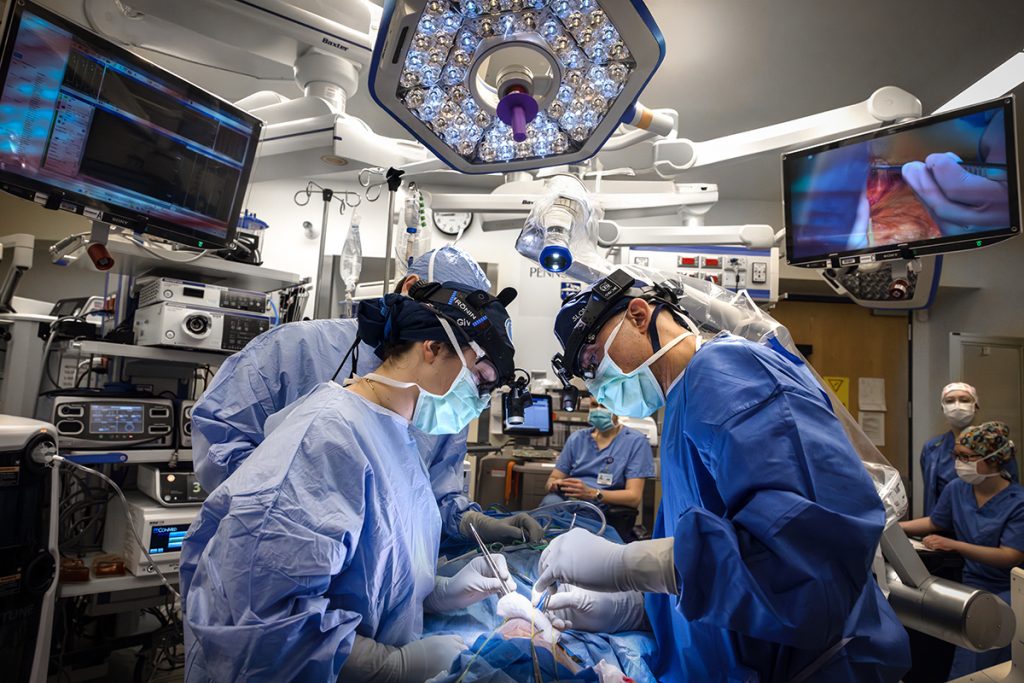
Dr. Guy Slonimsky, right, a head and neck surgical oncologist, and Dr. Alyssa Givens, a surgical resident, both with the Department of Otolaryngology – Head and Neck Surgery at Penn State Health Milton S. Hershey Medical Center, perform a Genio implant procedure to treat obstructive sleep apnea.
New Surgical Options
Neuromodulation, or the stimulation of nerve endings, is a newer procedure that changes how the tongue moves during sleep. The Genio device, approved by the U.S. Food and Drug Administration in 2025, joined Inspire therapy as a new way to stimulate nerves in the tongue to keep it in the right position. Both are outpatient surgeries and generally covered by insurance if patients meet the qualifications.
Goyal says these neuromodulation devices offer a major advantage over traditional surgeries.
“When you’re taking out the tonsils or tongue tissue, there’s a significant amount of pain and only a 50% to 60% rate of successful outcomes,” Goyal says. “The newer surgeries and implants have greatly reduced the pain component, and they have up to a 80% improvement in the frequency of sleep apnea events.”
Other Sleep Disorders
Other common sleep disorders include restless leg syndrome, sleepwalking and chronic insomnia – trouble falling or staying asleep for at least three months.
Some patients with chronic insomnia find relief from cognitive behavior therapy for insomnia (CBTI), a six-session protocol that addresses the behaviors and attitudes around sleep that can perpetuate insomnia. This therapy includes cognitive strategies, including cognitive restructuring, mindfulness techniques, and “constructive worry,” as well as behavioral strategies such as stimulus control and sleep restriction. Floyd says about half of patients who try CBTI experience substantial improvement.
Better Sleep Hacks
Good sleep habits can help everyone. Floyd recommends these five tips:
- Keep your bedroom dark, cool and quiet. Ideal temperature for sleep is 62-68 degrees. If you need sound, keep it to low. Limit outside light, and don’t use your phone 30 to 60 minutes before bed.
- Stick to a consistent schedule. Floyd says weekend wake and sleep times should remain within an hour of your weekday routine.
- Limit alcohol. Alcohol can increase sleep apnea episodes.
- Cut back on late caffeine and meals. Avoid caffeine later in the day and stop eating about three hours before bed. If you need a snack, choose something high in protein.
- If you can’t sleep, get out of bed. Do something relaxing like reading a book or putting together a puzzle in another room for 15 to 20 minutes, then try again. Don’t use this time to do chores. Relaxation is the goal.
Better sleep may start with small changes — but if you’re still tossing and turning, a doctor can help you get those zzz’s back on track.
Related content:
- The Medical Minute: Don’t snooze on sleep apnea
- The Medical Minute: Why am I always so tired?
- The Medical Minute: The causes and complications of snoring
Learn more about sleep medicine care at Penn State Health.
The Medical Minute is a weekly health news feature produced by Penn State Health. Articles feature the expertise of faculty, physicians and staff, and are designed to offer timely, relevant health information of interest to a broad audience.
If you're having trouble accessing this content, or would like it in another format, please email Penn State Health Marketing & Communications.
