Project ECHO spurs COVID-19 collaboration between health care providers across U.S.
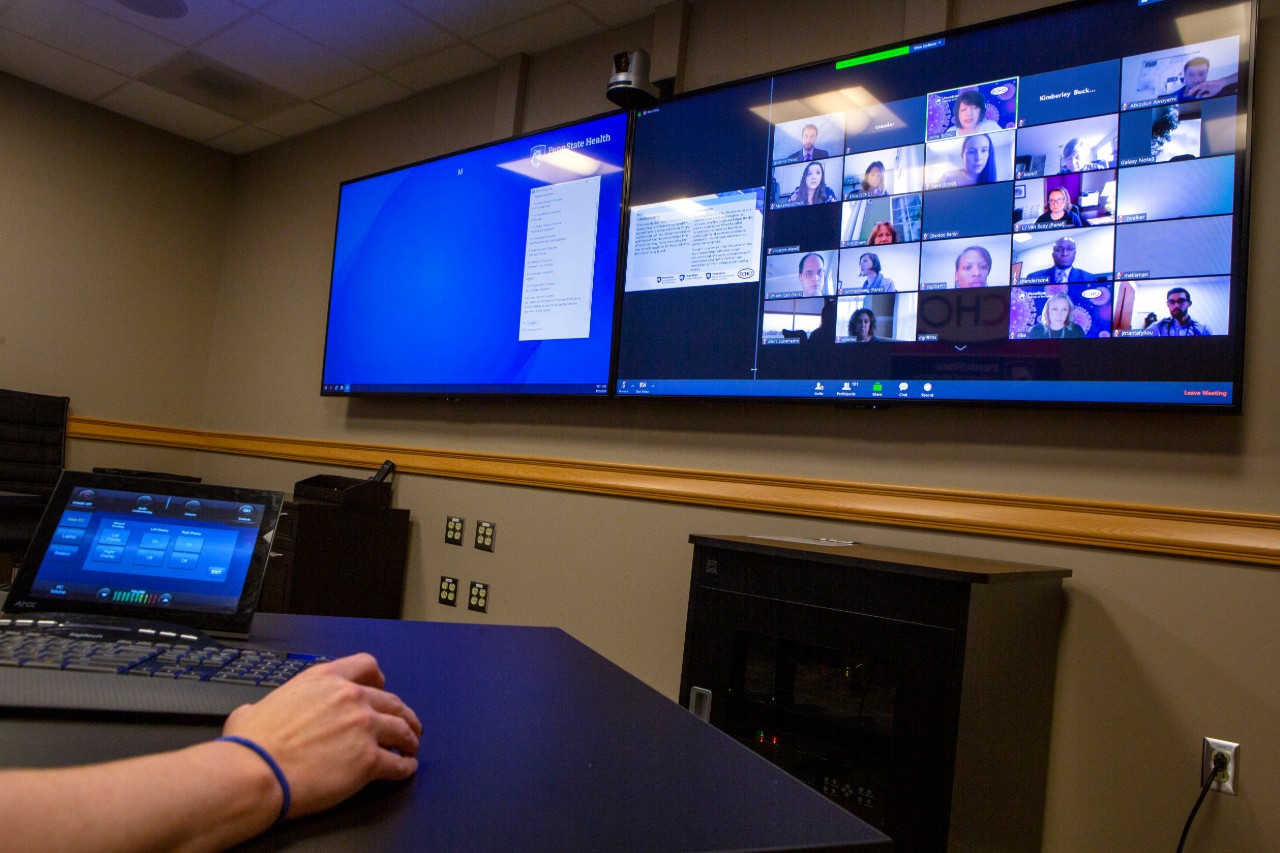
More than 100 health care providers gathered at their computer screens March 20 at clinics or hospitals hundreds of miles apart, at laptops on coffee tables or offices in their homes. They joined a broader discussion that might play an important role in addressing COVID-19.
It was Penn State Project ECHO’s (Extension for Community Healthcare Outcomes) first session in six weeks of programming surrounding the novel 2019 coronavirus. The hour-long online discussion offered more than a snapshot of the challenges providers face in the new normal — equipment shortages, the dire need for sterilization and protection from contamination. It also gave a hopeful glimpse into how the end of the pandemic might come to fruition — colleagues sharing knowledge, findings and real-time experience from the frontlines.
It’s the approach Project ECHO at Penn State has taken to a variety of issues since 2018. One Project ECHO program, for example, allows doctors to share strategies for treating patients with opioid use disorder. They discovered that many providers in rural areas lacked access to the level of training doctors in more urban settings received. Project ECHO has helped fill that gap.
“COVID-19 is completely different,” said Dr. Jennifer Kraschnewski, director of Project ECHO and associate professor of medicine and public health sciences at Penn State College of Medicine. “It’s like building an airplane while you’re flying it.”
And just how complicated the construction might be was apparent early in Friday’s discussion. Organizers presented a case study. A couple exhibiting mild symptoms but with no prior first-degree exposure to COVID-19 visited Northside Christian Health Center near Pittsburgh. Should they be tested?
“Yes,” one provider said. “It seems more important than ever to be doing as much testing as possible.”
“We don’t have enough tests,” said another.
“We are in a similar situation,” another provider agreed.
“We don’t have enough tests, and these are low priority,” said a third.
Other questions popped up about testing delivery drivers, co-workers, who should be tested and when. There were more questions than answers.
That’s not disconcerting, Kraschnewski said, because discussion is the point of introducing case studies during Project ECHO sessions. The deluge of questions they prompt (participants mostly submit their queries in writing to avoid a vocal traffic jam) can be answered offline, but case studies are all about helping one another find common ground. “That’s the secret sauce,” she said.
Another key ingredient on Friday came from Gavin Macgregor-Skinner, assistant professor in the Department of Public Health Sciences for Penn State World Campus’ Homeland Security program. He advised the group about personal protective equipment, disinfectant and how providers can protect themselves.
“You need to do your own risk assessment,” Macgregor-Skinner said. “You need to protect your eyes, nose and mouth.… You need to slow things down and do your own risk assessment.”
During the Ebola outbreak of 2014, Macgregor-Skinner helped train Nigerian health care workers. There, doctors and nurses battled an outbreak with scarce equipment. Protecting their own lives was of paramount importance but challenging and often requiring invention to ensure proper decontamination.
Macgregor-Skinner shared with the participants several strategies for reusing equipment when faced shortages. For example, it’s possible for doctors to wear same N95 respirator for multiple encounters with patients. The N95 respirator is a face mask that filters out airborne particles while allowing the wearer to breathe.
A provider can re-use the usually disposable face mask in a pinch, provided steps are taken to properly doff (remove) or don (refit) the mask. Two providers should never share respirators, he said.
Five additional session topics for the COVID-19 ECHO series will occur this week. The next discussion will cover Communicating with Family Members and Visitors. It’s scheduled for Thursday, March 26, at 8 a.m. Please email echo@psu.edu for more information.
Nearly 200 health care workers have signed up for the series in less than 24 hours.
“Knowledge is literally changing daily,” Macgregor-Skinner said.
If you're having trouble accessing this content, or would like it in another format, please email Penn State Health Marketing & Communications.
