St. Joseph nurse-driven mobility program delivers for COVID-19 patients
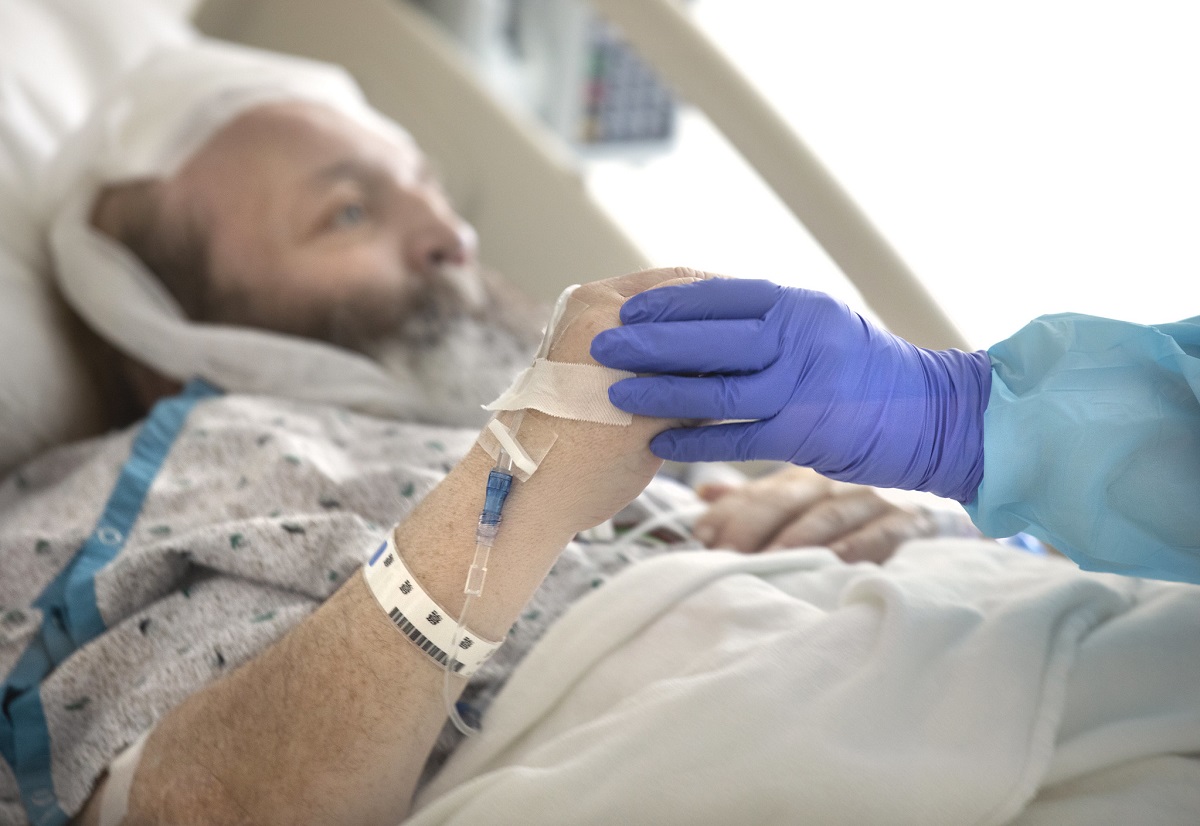
At St. Joseph Medical Center, a new program geared to get COVID-19 patients moving to help their recovery is bearing fruit.
In the eight weeks since St. Joseph Medical Center rolled out its Stay Active, Stay Strong program, nurses have witnessed improvements in patient activity levels while deconditioning and isolation have decreased.
“In a normal world, the patients would have more interaction, staff from a variety of departments would be in and out of the rooms and their activity levels would be different,” said Sharon Strohecker, vice president of clinical services and chief nursing officer. “These patients aren’t having that normal experience. They are isolated. The doors are shut. No family is coming in. Even the nurses, who are donned head to toe in personal protective equipment, are spending less time in the patient space.”
Strohecker asked Shelley Hickey, a nurse educator, to develop an evidenced-based mobility team that would make a difference for patients.
“When I began to research similar mobility programs, I found the majority were driven by physical therapy departments,” Hickey said. “What is unique about this program is that it is nurse-driven yet partners with physical and occupational therapy.”
Hickey created operational and educational elements and, together with Jo Rivera, a registered nurse, launched a program to visit every patient in the unit once or even twice a day, Strohecker said.
Point at the image below to reveal slideshow player controls.

The program relies on the nurse and clinical associate team of Rivera and Hannah Schmidt to make 10 to 15-minute visits, during which they educate patients on the importance of keeping active. Rivera and Schmidt help the patient complete appropriate exercises, such as passive and active range of motion, isometrics and working with assistive devices.
“The patients are loving it. Their activity levels are better, they are stronger and out of bed more frequently,” Strohecker said.
“Patients who are considered independent are asked to perform the exercises as instructed. We also encourage them to be out of bed to eat their meals,” Rivera said. “We want them up and moving. Sitting in a chair really helps their lungs expand to move air through and get their lungs healthier.”
The program has been successful in part due to it involving physical and occupational therapists and the bedside nurse.
“We communicate daily before visiting patients on the COVID unit to ensure all staff involved are aware of any patient needs or concerns,” Rivera said. “If we know therapy will be in the patient’s room in the morning, we plan our visit in the afternoon so we don’t overwhelm the patient with activity.”
Rivera also worked with the Therapy Department to develop a series of exercises patients can do on their own up to four times a day. Posted in their rooms, they serve as a reminder that activity helps build strength.
“Sometimes we walk by their rooms and see them doing the exercises,” Schmidt said. “Also, the dietitian said she sees an improvement in patients getting up and sitting on the side of the bed to eat.”
Hickey and her team are still compiling data to determine if the program has had a positive effect on the average length of stay. That’s a goal of the program — average stays at St. Joseph have significantly increased because of the longer recovery phase for COVID-19 patients. But the positive response to the program from patients is enough to know they are headed in the right direction.
“Our patients say it feels good to have their feet or arms exercised, to get out of bed, stand or walk. They also enjoy the socializing that comes along with the daily visits,” Rivera said. “Not all COVID patients need physical and occupational therapy, but every COVID patient benefits from mobility.”
If you're having trouble accessing this content, or would like it in another format, please email Penn State Health Marketing & Communications.
