Ask Us Anything About… RSV in Children
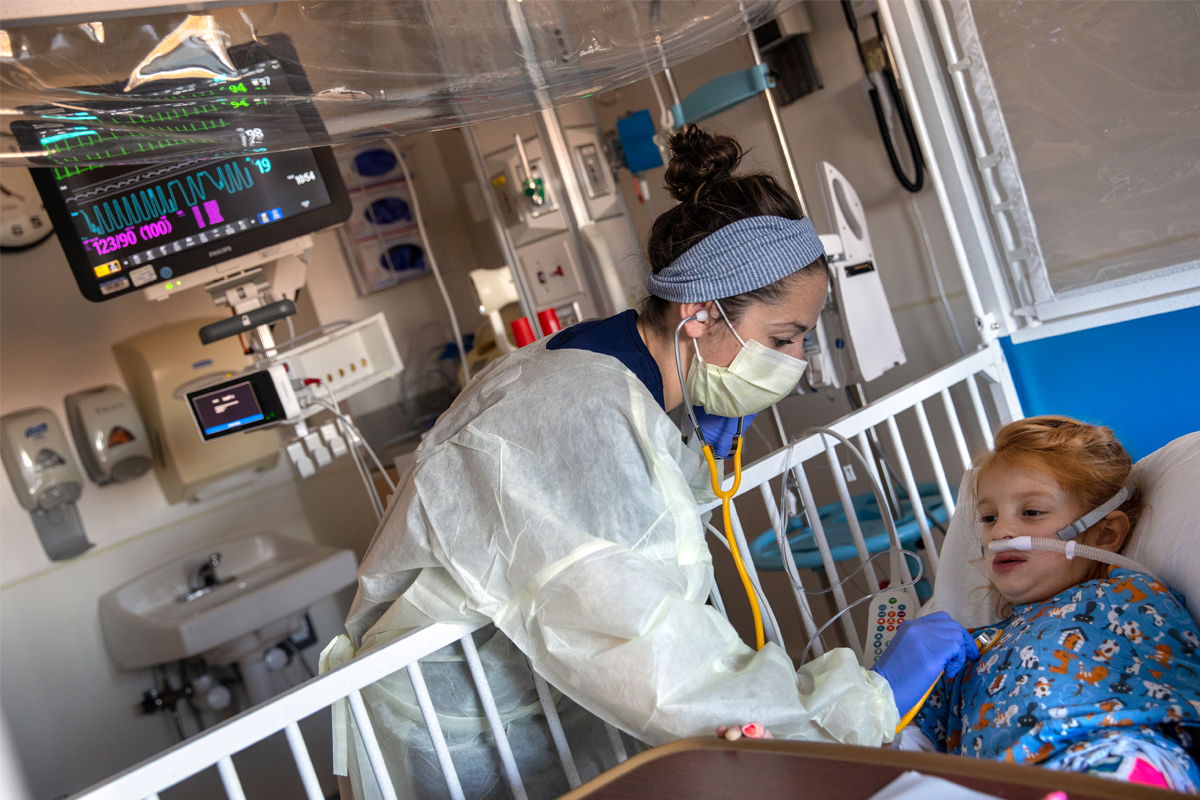
We’ve been hearing a lot about RSV — or respiratory syncytial virus — lately. While cases are reported every year, an early influx of cases — and of hospitalizations, including among children — is adding to concern this year. We find out what parents need to know from Dr. Jessica Ericson, a pediatric infectious diseases physician, and Dr. Duane Williams, a pediatric critical care physician — both of Penn State Health Children’s Hospital.
View full transcript of videoTranscript
Scott Gilbert – RSV in Children. I’m Scott Gilbert. We’ve been hearing a lot about RSV lately, haven’t we? It stands for respiratory syncytial virus. And while cases are reported every year, an early influx of cases and of hospitalizations, including among children, is adding to the concern this year. To alleviate some concerns and to provide parents with answers, we have a couple experts with us today, including Dr. Jessica Ericson. She’s a pediatric infectious diseases physician at Penn State Health Children’s Hospital. And Dr. Duane Williams, a pediatric critical care physician at Penn State Health Children’s Hospital. My thanks to both of you for being here today. Well, Dr. Ericson, let’s start with the symptoms of RSV. Because, let’s face it, in the winter, there are a lot of respiratory illnesses that circulate, especially in children. What are some of the symptoms of this?
Dr. Jessica Ericson – So most of the time, RSV is going to look just like any other respiratory virus, like you said, Scott. So, runny coughing, sore throat, sometimes fever, sometimes headache, body aches. The big thing that makes RSV different is that it can cause more often, lower respiratory tract infection. Usually that’s seen in little babies or smaller toddlers, where that coughing progresses to difficulty breathing. These children may be breathing faster, be breathing harder, sometimes need oxygen or other kinds of help with breathing.
Scott Gilbert – Now, Dr. Williams, you work in the pediatric intensive care unit at our children’s hospital. Take us behind the scenes there. Because we’re hearing a lot about RSV driving high-patient volumes at children’s hospitals across the country. We’re seeing that in Hershey, aren’t we?
Dr. Duane Williams – Yeah. Yes, sir. You know, we’re sharing in the ask to serve people and their little ones in our unit as well with the increasing volume. And when these kids come in, just like Dr. Ericson said, it’s usually because that work of breathing has gotten past the point of what could be taken care of at home. So they come into our unit and into our facilities and we look to help to support their work of breathing, help with their, you know, clearing some of that mucus that’s causing a lot of their symptoms to get them home as fast as we can.
Scott Gilbert – And so what are some of the therapies then, Dr. Williams, that a child, when they’re admitted to the children’s hospital, what are some of those treatments and therapies specifically that they may undergo?
Dr. Duane Williams – Yeah. So in some of our children, it’s really clearing their airways. We have just different tools that we have within a hospital that we can do that to help these little ones out. The other aspect is, if they share some other symptoms of other illnesses or there’s a strong family history, there’s some dilating — bronchodilating — medicines that we try at times. But the biggest thing that we’re doing is really supporting their work of breathing through different devices like high-flow nasal cannula, pressure devices over their mouth and nose. It just really helps them so they don’t have to work as hard to breathe. And in some instances, even what we call invasive mechanical ventilation. So having to help these little ones out with the breathing tube to support their work of breathing until they’re able to work through the virus.
Scott Gilbert – You’re watching Ask Us Anything About RSV in Children from Penn State Health. With us are two physicians from Penn State Health Children’s Hospital, Dr. Duane Williams and Dr. Jessica Ericson. We welcome your comments, your questions for them in the comment field of this Facebook post. Whether you’re watching this interview live or even after the fact, feel free to add those comments and questions, and we’ll be sure to engage with you and get you some answers. You know, Dr. Ericson, parents must wonder, given how similar these symptoms of RSV are to some other illnesses, how do they know when their child can probably recover at home versus when medical care is needed?
Dr. Jessica Ericson – Thankfully, the answer is the same, whatever the virus is. So it’s not particularly important that parents know whether their child has RSV or another virus. The important thing is to look at your child and what they’re doing. If they’re laying around, they can’t eat, they can’t drink, they’re spending all of their energy focused on breathing, that would be a child who probably needs a little bit of help to get through the worst of the illness.
Scott Gilbert – And there are a lot of choices, of course, of places to receive care. There’s the pediatrician’s office. There’s also telehealth. But there’s also urgent care and a hospital emergency department. I mean, I guess, how do you determine what level of of care is needed? I guess, it all goes back to that very simple question. Are they having trouble breathing, right?
Dr. Jessica Ericson – Yeah, that’s exactly right. So the things that you would see that would tell you that your child is having a lot of trouble breathing are seeing their belly or chest moving up and down while they’re breathing. Sometimes the skin will suck in around the collarbone or between the ribs. Those would all be clues that the child is having more trouble breathing. And that would be a time to consider taking them into the emergency department or an urgent care. If it’s more limited to cough, runny nose, even if that cough lasts a long time, that would be a time to see your pediatrician or give your pediatrician’s office a call and see what they think would be the best place for your child to be taken care of.
Scott Gilbert – That’s some great advice, because I’m sure we don’t want to drive people directly to the hospital emergency department at the first sign of a cold. But at the same time, we don’t want to deter them from going there if their child has severe symptoms, right?
Dr. Duane Williams – Yeah, I think that’s really important. I think the great thing about kids — and, you know, we’re kid doctors, so we love kids — is they love to play, right? Your kids love to play. And they’re going to play through so many things. And when you see things that are affecting them from playing — I think Dr. Ericson said it greatly, they’re just sitting around, right? I think when you see them just sitting around, not being able to drink, I use the wet diaper test. You know, if your wet diapers are not the same as you’re normally used to seeing, you know, the combination of dehydration and the willingness not to play, those are when things become really concerning. And that’s when you thinking, do I need that emergency room to look at my little one? I think partnering with your pediatrician is always that first best bet. Give them a call. Tell them what you’re seeing. But that’s when those kids get into trouble. I don’t want to play, and I’m not drinking as well, I’m not eating as well.
Scott Gilbert – That’s great advice. You’re watching Ask Us Anything About RSV in Children. We welcome your questions for Dr. Duane Williams and Dr. Jessica Ericson. Just drop them in the comment section and we’ll bring them up on the screen. Here we have a great question from Ashley. I’m curious for the answer to this one myself. Once a child has recovered from RSV, are there any natural immunities for a timeframe? So I think she’s saying, for a certain period of time afterward, are they therefore immune from getting it again?
Dr. Jessica Ericson – The short answer is we’re not entirely sure. But in reality, you probably have some amount of immunity from the immune system responding to that virus for several weeks. We do definitely see some children who get RSV more than once in a winter. So it, unfortunately, doesn’t give you long-lasting immunity. So the sort of usual advice to stay away from sick people, to wash your hands well, that’s going to continue to be important even after you’ve had a bout with RSV, because it doesn’t really give you long-lasting immune protection, more than really just a couple weeks.
Scott Gilbert – And Ashley has another good question here. I’m liking her questions more than mine. If a grandparent tests positive for RSV, how long should we wait for them to be around our kids? Like, how long is someone contagious? And I would say the inverse is probably true as well. Because we should remember, seniors and immunocompromised people are among those who are also at risk for RSV. But, Dr. Williams, what kind of advice would you have for Ashley with regard to that type of thing?
Dr. Duane Williams – Yeah, and this one is also difficult because — with Dr. Ericson — is saying that yes, RSV causes infections in kids and it looks a certain way, but then there’s also other viruses that look the same way. And then kids, at times, will recover from one and then get another. We’re actually seeing that in a lot of our kids. And so when you see the absence of symptoms, that’s a really good sign that we’re comfortable being around others. And then there’s differences in timeframe as far as it pertains to the actual virus. And, you know, the the rule of thumb is somewhere between five to seven days of not having symptoms. But I don’t know, Dr. Ericson, what would you say is that accurate timeframe from the really I’m not seeing any symptoms anymore and therefore, you know, we can interact and engage with loved ones?
Dr. Jessica Ericson – Yeah. Part of the reason that it’s hard to answer that question and just say, well, it’s 10 days, is because it’s an average. So some children will stop being contagious after just a few days, four, five, seven days. And some children, especially those who’ve been really sick, they might actually be contagious for two or three weeks. So kind of the best way to guess if your child is contagious still or not is with the symptoms. And once the symptoms are gone, the longer the symptoms have gone, the less likely they are that they’re still going to be contagious.
Scott Gilbert – Good advice there. Dr. Ericson, some health experts say that the lack of exposure to viruses from the last couple years, you know, due to masking, social distancing, keeping kids home from school, has led to a now sudden spike in exposure with the easing of these measures. Basically, saying we’ve been shielding kids from viruses, and now, all of a sudden, they’re exposed to them. Is there some truth to that? Do you buy into that?
Dr. Jessica Ericson – Well, it kind of depends a little bit on what you mean by that. So I don’t think that we have evidence that these children’s immune systems work less well because of their experiences over the last two years. But what is true is that we didn’t have really any kids in the hospital for RSV for the last two years. So now we have three years’ worth of children who are needing RSV for the first time this year. And so we have some children who would have been hospitalized on their first time in 2020. And some kids who would have been hospitalized on their first time in 2021. And they’re now all meeting RSV for the first time in 2023. So I think that it’s a math problem that’s coming to cause problems with so many kids being sick at the same time. But there’s not really any evidence that it’s because we have a bunch of kids whose immune systems don’t work anymore. There’s not evidence that that’s playing a role here.
Scott Gilbert – We’re hearing a lot about RSV lately, and that’s why we’re getting some good advice today from Dr. Jessica Ericson and Dr. Duane Williams from Penn State Health Children’s Hospital. This is Ask Us Anything About RSV in children. We welcome your questions in the comment field below this Facebook post, and we’ll make sure that we get the answer to you whether you’re watching this interview live or even after the fact, we’ll respond in the form of a comment. So Dr. Williams, from a hospital perspective — again, I know this is not unique to Penn State Health Children’s Hospital. It’s being seen across the country. But this kind of pseudo collision we’re seeing right now between RSV, flu, some COVID-19, how much does that all factor together in terms of their cumulative effect?
Dr. Duane Williams – Yeah, I think that’s a question. You know, what we’re seeing — and you know, we’re partnering with, you know, we’re gaining insight from other institutions across the country who are, you know, working really hard to serve as many children and families as possible. And we’re not alone, and, you know, really operationalize how can we care for these kids? So what we’ve done here is really trying to get our kids into the location where they’ll get the care that they need to recover and get home. And we’ve augmented a lot of what we’re able to do here at the Children’s Hospital. I’m grateful to see the selflessness of nursing and respiratory therapy and our environmental health team, our residents, and our faculty, just coming together trying to get these little ones home. So we’ve used every space that we possibly can, as other children’s hospitals across the country are doing as well. Really trying to serve the children in our region and get them home safe.
Scott Gilbert – And I think you actually just addressed part of Josh’s question. We’ll bring it up on the screen here and see if either of you have anything else to add. But Josh is asking, we continue to hear how hospitals are stressed with all these viruses circulating. How is Penn State Health prepared for the influx of children? And should parents be concerned there will not be room to help their child? From what I’m hearing, Dr. Williams, it sounds like some really innovative efforts are underway and some great teamwork is underway to try to prevent any kind of scenario like that. But, at the same time, you know, we do have to be flexible from a care perspective.
Dr. Duane Williams – Yeah. So we are using the breath of Penn State Health in order to meet the needs of our children in our region. And these are our kids. So we really want to extend all the possibilities that we can to meet these needs. We are humbled. People will trust us with their kids. And we want to do that. And then we also look and learn from others who are facing this as well through the country. You know, what are they doing in order to meet the needs of these little ones that people hand to us for their care?
Scott Gilbert – Well said. Dr. Ericson, we, of course, have vaccines. They’re safe and effective for the flu and for COVID-19. No vaccine yet for RSV. Any news on the horizon there, any possibilities in the works?
Dr. Jessica Ericson – Well, I sure hope so. We’ve been working on a vaccine for RSV for decades, and there have been a few that have made it pretty far in clinical trials. So fingers crossed, maybe in the next three years or so, we’ll start to have that available. That will be an important vaccine both for the elderly and for young babies and children. So we’re hopeful that that will be an option to help us deal with this issue that’s to some extent a problem every year.
Scott Gilbert – Yeah. And does the prevalence, Dr. Ericson, of something like RSV make it important that people get vaccinated for the ones that we do have a vaccine for — the flu and COVID-19? Again, when we think about all of us doing our part to try to not overload hospitals.
Dr. Jessica Ericson – Yeah, absolutely. So both the COVID vaccine and the influenza vaccine are less good than we would like at keeping you from getting sick at all. But they’re both very good at keeping people from getting really sick and from ending up in the hospital. So they’re a great way to bring the total number of people who need to be in the hospital down. And that’s really helpful at a time when we’re really operating at the the edge of how much we’re able to handle.
Scott Gilbert – And, Dr. Williams, anything to add to that, again, from the hospital perspective and from somebody who’s really trying to balance things here?
Dr. Duane Williams – Yeah, I think — just to echo those comments — you know, we’re trying to make space for as many little ones as we can. And I think the reason why this time — I think Dr. Erikson spoke to it earlier — is we’re actually seeing it in older kids with RSV. Older kids with some of these other viruses that wouldn’t normally have been admitted for it. I think that speaks to, like she said, they just haven’t been exposed to it before. So for those other means that we can help these little ones and sometimes even bigger ones be able to, even though they do get sick, but be able to stay at home and be cared for at home, it’s going to be really impactful. So we have the means to support as many kids as we can.
Scott Gilbert – You’re watching Ask Us Anything About RSV in Children from Penn State Health. I’m Scott Gilbert, alongside Dr. Jessica Ericson and Dr. Duane Williams. They have some great information here. So feel free to add your comments, your questions in the comment field of this Facebook post, and we’ll get those questions answered for you. And if you find this content valuable, as we hope you do, click on that share button. Share with your network, so we can help to get the information out there about how everybody can hopefully do their part to try to stay healthy. And, you know, as I think about that, I think about prevention. Dr. Ericson, what is the best way; what are some of the best ways to prevent RSV? I’m guessing, we’ve heard some of these tips before, haven’t we?
Dr. Jessica Ericson – Yeah. I think the best tip from a community standpoint is that if you’re feeling sick, if your child is feeling sick — coughing, runny nose, fever — stay at home, skip the birthday party, stay home from school, stay home from work. If you’re not able to, then be extra vigilant about hand washing. If you have to go out while you’re ill, that would be the perfect time to wear a mask, to keep your germs to yourself as much as possible. And then, on the other side, if you’re feeling healthy, then good hand washing, you know, doing activities outside and those kinds of things can be really helpful.
Scott Gilbert – You know, Dr. Ericson, given the fact that — I’ve seen some media reports recently that RSV may be receding in some parts of the US. For example, the Southeast, and also some mountainous parts of the West. Is that cause for even conscious optimism here in Pennsylvania?
Dr. Jessica Ericson – I think possibly. So RSV does start in the South and then move North. So we would expect that whatever RSV is doing in the South of the country will be what it’s doing here in another weeks. But the reality is is we don’t really know what the RSV season looks like anymore. Three, four years ago, we would say RSV comes October to March. And with really having none for the last two years, we’re kind of starting over with figuring out what an RSV season looks like. So it may be that we take a break, have fewer cases for November, and then it comes right back in December. We just really don’t know what RSV season looks like anymore. But, yeah, I’d say that’s a hopeful sign, since what happens in the South, you know, goes North. So hopefully we will see that here soon.
Scott Gilbert – Well, that’s good to hear. And, of course, it’s also good to know that RSV is not new. You know, physicians know how to treat it. In fact, there’s a lot of good information on the Centers for Disease Control and Prevention website. We’ll be sure to share a link in the chat of this Facebook post so that folks have the direct link to those resources. But I want to thank you both. Dr. Jessica Ericson, she’s an infectious diseases physician at Penn State Health Children’s Hospital. Dr. Duane Williams is a pediatric critical care physician at the Children’s Hospital. Thanks so much to both of you for your time. And thanks to all of our viewers. And for the great questions here, for Ask Us Anything About RSV in Children from Penn State Health.
Collapse TranscriptMore AUAAs
If you're having trouble accessing this content, or would like it in another format, please email Penn State Health Marketing & Communications.
