Ask Us Anything About…NICU Care
When having a baby, parents don’t like to imagine their child needing to stay in the neonatal intensive care unit (NICU). Dr. Jeff Kaiser, chief of neonatal-perinatal medicine at Penn State Health Children’s Hospital, helps new parents understand what they need to consider when choosing a hospital and what to expect if your child needs to go to the NICU.
View full transcript of videoTranscript
Scott Gilbert – From Penn State Health, this is Ask Us Anything About NICU Care. I’m Scott Gilbert. When parents-to-be are thinking through all of those details from the color scheme of baby’s room to where they want to deliver, they often do so with the expectation that their baby will be born healthy, but sometimes newborns need special care. In fact, it takes a team to provide that type of care to complex and critically ill newborns. Such a team of health professionals staffs the neonatal intensive care unit, or NICU, at Penn State Health Children’s Hospital, and here to give us an inside look at this unit and to talk about NICU care in general is Dr. Jeff Kaiser. He is Chief of Neonatal and Perinatal Medicine at Penn State Health Children’s Hospital. Dr. Kaiser, good to have you with us today.
Dr. Jeff Kaiser – Thanks, Scott.
Scott Gilbert – So when — Dr. Kaiser, when new moms are thinking about where they want to deliver like I mentioned, they don’t always take a hospital’s NICU into consideration but what is a NICU? Let’s start there and why it’s so important to think about when choosing where you want to deliver.
Dr. Jeff Kaiser – Sure. So NICU stands for neonatal intensive care unit. No one thinks that they’re going to deliver early or their baby’s going to have a problem, but when that happens, maybe one to 10% of the time, it’s good to know that there’s insurance right after they deliver and we’re the insurance. If a baby is born early, we’re at the delivery. If the baby has breathing problems, we have ventilators. We are there for when things go wrong. And a lot of times people always prepare for the worst. Well, we are that insurance to help.
Scott Gilbert – Yeah. And so give us an idea of which babies end up in the NICU and some of those specific conditions that a NICU care team cares for.
Dr. Jeff Kaiser – Sure. So one of the most common things is prematurity. So full term is considered 37 weeks or used to be called 9 months. We have babies come as early as 23 weeks, so we’re talking about 17 weeks or 4 months early. That’s a common thing. A lot of times we actually have babies that are not quite term. They’re smaller and they’re not very good at eating, so they’ll stay with us. We have babies with heart problems that need surgery. We have babies born with intestines that are twisted or on the outside. We have babies who actually have high blood pressure in their lungs and they need special ventilators or special gases or even sometimes we do something called ECMO. It’s like a cardio pulmonary bypass machine. We can do it right in the NICU and that just saves lots of lives.
Scott Gilbert – Right. So when a baby is born prematurely, it sounds like you’re saying a lot of systems are affected, how they breathe, their hearts, their digestive systems. Is that a fair assumption?
Dr. Jeff Kaiser – Exactly. Exactly. The thing that kind of presents itself right away is breathing and so sometimes we have to put them on ventilators. When they’re immature, they’re not very good at eating and their intestines are immature. And then premature babies, just because they’re premature, their immune systems are premature, they’re more likely to get infections, so those are some of the issues that we have to deal with.
Scott Gilbert – You’re watching Ask Us Anything About NICU care from Penn State Health. I’m Scott Gilbert alongside Dr. Jeff Kaiser. He is Chief of Neonatal Perinatal Medicine at Penn State Health Children’s Hospital and we’re talking with him to kind of demystify what happens in a NICU because again, it’s one of those places that we often as parents or as expectant parents don’t expect our child to end up, but for very good reason they do receive care there sometimes, and we’re trying to kind of learn more about that kind of care. And so there are lot of intensive care units in a hospital and Dr. Kaiser, in a children’s hospital, there’s also a pediatric intensive care unit, but there’s a difference there, right? Is it as simple as children of a certain age are cared for in each type of unit, or is it a little deeper than that?
Dr. Jeff Kaiser – It’s a little deeper. For the most part, pediatric intensive care, the PICU, they can actually take care of babies as young as newborns all the way to 18 year olds. We on the other hand, take care of newborns maybe up to 6 months or so. If they have specific problems that are not neonatal, like for instance, if there’s a car accident, they are better served in a pediatric ICU.
Scott Gilbert – All right. The 56-bed NICU at Penn State Health Children’s Hospital and we should mention it just moved into the expanded portion of the Children’s Hospital. That was just a few weeks ago, very exciting time in our children’s hospital to be able to bring that into the freestanding building. Well that NICU is the region’s only level 4 NICU. We say that a lot, but to a parent, what does that mean. Why does that matter?
Dr. Jeff Kaiser – Sure. So level 4 is the highest level according to the American Academy of Pediatrics. So level 1 would be just a newborn nursery. Level 2, they can keep some babies maybe that need a little bit of oxygen. Level 3 NICUs can keep some babies on ventilators, but a level 4 NICU can do everything. We can do surgery 24/7. We have every kind of ventilator, every kind of high risk procedure, we can do in our neonatal ICU and there are only three in Pennsylvania. There’s Philadelphia. There’s Pittsburg, and then there’s Central Pennsylvania, and that’s us.
Scott Gilbert – So, we welcome your questions for Dr. Kaiser here. Again, this is Ask Us Anything About NICU care from Penn State Health. You may be an expectant mother with some questions about this type of care, and again, why it matters in that choice of a place to give birth and that’s why we’re here today, so feel free to add those questions in the comment field below this Facebook post, whether you’re watching this interview live or if you’re watching it on playback after the fact. So the design of the NICU in the newly expanded children’s hospital takes into account the latest research but also input from families here in central Pennsylvania. Can you take us behind the curtain and tell us a bit about what that design process looked like?
Dr. Jeff Kaiser – Sure. Sure. So if you can imagine a baby about two feet, they’re in a room. Most of our rooms are single rooms or rooms for twins or we have one room for triplets. These rooms are single-family rooms, so family, mom and dad, can stay with their baby from the time of admission to the time that they’re ready to go home. So most NICUs around the country, most new ones, are just single room NICUs, but we learned within the last two or three years that babies that stay in single rooms by themselves, and their parents cannot stay because they have other — they have to take care of other children or they have work or other reasons why they’re not there, those babies don’t hear enough human voice and it turns out that hearing adult words, human voices, really important for their development. So for those babies that start in these single rooms and their parents cannot stay, once they’re breathing on their own and eating on their own, we’re actually moving them to one of three rooms that have six beds. And those rooms have six beds, you know, they’ll have five other patients, five other families, several nurses. They will hear a lot of human voice and based upon our new model, our babies are going to have the best possible long-term outcome simply because of our new bed structure. So we call it a hybrid bed structure and we’re one of the first that has that in the U.S.
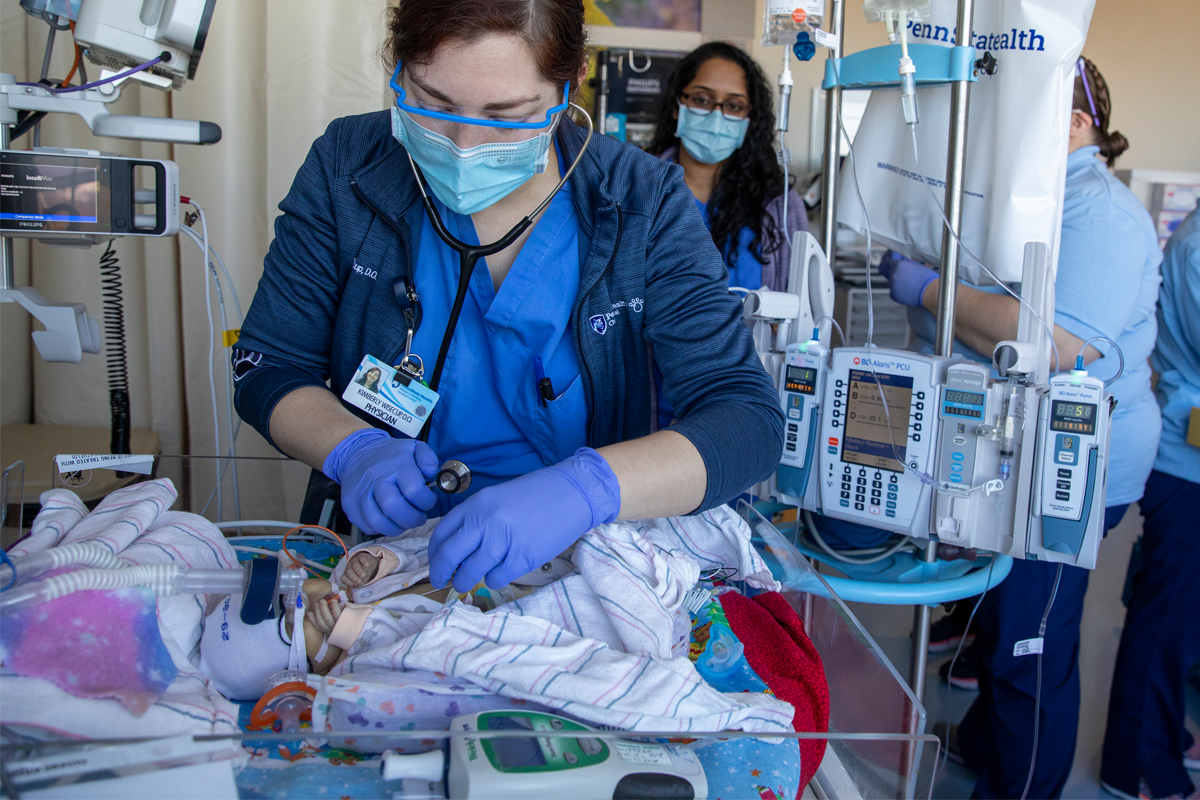
Scott Gilbert – Very interesting. So, you know, Dr. Kaiser, I have to say, when people picture a baby in a NICU, the initial picture they get in their mind is one of a lot of wires and tubes and that can be scary. That can be a little daunting, especially for an expectant parent to think about. What are some of the more common types of equipment used in the NICU? Can you help to demystify some of those wires and tubes for us?
Dr. Jeff Kaiser – Sure. Sure. Well, the first thing is I’m so impressed. Parents can walk into a room and their baby is hooked up to every monitor, is on a ventilator, and they don’t see all of that. They see their baby. It’s really quite amazing that they can focus that way, but we’ll have babies like in the picture right there. That baby has air being pushed into the nose using something called CPAP. Sometimes they have breathing tubes in their mouths that go down to their lungs. They’re connected. We have leads on their chest so we can see what their heart rate is. We have monitors that are on their fingers that how much — tell us how much oxygen is there. So a baby can be hooked up to a variety of things. Oh, in addition, they have IVs where they’re getting fluid and medications, so they can have 10 or 15 or 20 different plastic connections but parents see their baby. It’s just so incredible that they look past all of that. But our nurses are really great at kind of demystifying all of that and they explain what everything is and they explain what the cardiorespiratory monitor is and while it’s really good to see the baby’s heart rate, it’s such a sensitive monitor that it kind of makes people crazy when they look at it too much, so our nurses really make it — make parents understand that when it looks like the baby’s heart rate is low, we actually look at the baby and if the baby’s pink, they’re fine. So our nurses are fabulous at kind of explaining all of that and making it just very clear for patients — for parents, I’m sorry.
Scott Gilbert – That’s great. To take parents along that care journey, I’m sure is so important to make sure that they’re involved very step of the way.
Dr. Jeff Kaiser – It is. It is. You know, and there’s been lots of research over the last 15 years or so that with these single rooms where parents do stay, the most important thing that’s associated with a good long-term outcome is parents literally being there. It’s not just a ventilator. It’s just not the nutrition. It’s parents being there talking to their child, learning how to give some of the care, change diapers. When parents stay there and they’re comfortable, parents go home feeling more comfortable. The baby just ends up doing better and these are long-term outcomes, two years, five years. Really and our NICU’s now set up to allow this parent participation that is just so key to the long-term outcome. There’s another really cool thing that parents do. We’ll have babies as small as one pound and they have the breathing tube in their mouth and they’re hooked to a ventilator, yet we will pick up that baby and place that baby still on a ventilator on a parent’s chest. We call that skin to skin. Even when that baby is a pound or less, that skin to skin, that participation with their parents have huge important benefits for the children and again, the more skin to skin that’s done, the better long-term outcomes there are. So our nurses and respiratory therapists work together with the parents to allow this to happen, early on maybe once a day, but then later on as often as possible.
Scott Gilbert – What questions do you have about a NICU? This is a great time to get those answered from Dr. Jeff Kaiser. He’s Chief of Neonatal and Perinatal Medicine at Penn State Health Children’s Hospital and he’s our guest today for Ask Us Anything About NICU Care. So feel free to add those questions to the comment field below this Facebook post here. Another question I have, and, you know, you’ve talked a little bit about nurses and doctors and I know that when we think about a hospital unit, that’s what we think about, right? We think of nurses and doctors and some of the other staff, but in a NICU, there is a really huge team behind the scenes that’s involved with the care of each patient, right?
Dr. Jeff Kaiser – Yup. So it’s incredible the amount of people that take care of a one-pound baby. Then you have your neonatologist, the doctor. You have the bedside nurse, and that bedside nurse is probably one of the other most important things about long-term outcomes. They spend 24/7 at the bedside with that baby. Unfortunately, the doctors can’t because we may have 20 patients. So we have some of the best nurses that are attuned to small babies. We have pharmacists that are specialists with baby medications. We have dieticians. We have child life that help us with positioning babies. We have milk lab technicians. We used to have a milk lab in the basement of the hospital, now it’s up in the NICU. We have social workers. We have care coordinators. And very importantly for when babies are on ventilators, we have some of the best respiratory — baby respiratherapists I’ve ever met in my whole career that they work with us to help us decide what best ventilator, how to wean the baby from the ventilator, and when to take the baby off the ventilator when things are going great. It takes a village to take care of a baby.
Scott Gilbert – And just like you’re describing here, I mean, the NICU team doesn’t exist on an island. It’s really the opposite. I mean, they collaborate with other teams across the children’s hospital and the health system and I think that’s part of the thinking behind what we refer to as the perinatal center, right? Can you tell us a bit —
Dr. Jeff Kaiser – Yup.
Scott Gilbert – — about that?
Dr. Jeff Kaiser – So the perinatal center is a group that’s a consortium of many services in the hospital. So it starts off with obstetrics and maternal fetal medicine, neonatology, and then a variety of pediatric specialists such as pediatric cardiologists, pediatric nephrologists, pediatric infectious disease doctors. So when it is found out that a family has a pregnancy where there may be a problem, care is transferred to Penn State to the perinatal center so you get the care of the pregnancy from all sides. Now the maternal fetal doctors or the high-risk obstetricians’ kind of take the lead on this. But most of these babies end up coming to the NICU. We meet the parents before the delivery. We talk about all of the different possibilities. This perinatal center really demystifies having a baby that you know is going to have a problem. And you can find a lot of information about it on the website looking up Penn State perinatal center. One of the other really cool things about our NICU now is it used to be in the adult hospital and we were far away from labor and delivery, also in the adult hospital. So one of the very nice things about our NICU is we’re on the eighth floor. We’re on the top floor. But labor and delivery, they actually moved to the children’s hospital on the seventh floor, so that allows us to have much better collaboration. We’re literally 10 seconds away by running down the stairs so if labor and delivery is having a problem with a sick baby or a mom, we’re right there, and that’s different from most other children’s hospitals in the country, just that excellent collaboration and just being so close to our obstetrical colleagues.
Scott Gilbert – So I’m sure it’s not always possible to foresee problems sometimes but it sounds like the purpose of the perinatal team is to approach each baby with a collaborative — kind of a collaborative approach to make sure that you try to foresee any problems as much as possible prior to birth.
Dr. Jeff Kaiser – Correct. And thanks for saying that, Scott. But it also allows the plan for delivery, whether they’re going to deliver whenever they go into labor or deliver at 37 weeks, the neonatologist again, will meet with these families before delivery and kind of demystify what it is going to a NICU. But I guess the other great thing is we have the specialists. We have the cardiologist who you can speak to. We have the cardiovascular surgeon who you can speak to. It just decreases the stress of knowing that you have a baby who may have a problem.
Scott Gilbert – So Dr. Kaiser, a lot of expecting mothers are probably nervous about COVID-19, especially when it comes to delivery. What are some of the things your team is doing to help keep our tiniest patients safe here in the midst of the pandemic?
Dr. Jeff Kaiser – So we have worked very closely with our obstetrical colleagues and with the whole children’s hospital about what to do especially when a mom comes in who’s COVID positive or who is suspected to be COVID positive. Initially, when the baby is born, we will do something called delayed cord clamping. We actually will allow the placental blood to flow into the baby for one minute. We’ll then clamp that cord, take care of the baby and move that baby out of the room. And if a mom is in labor, we make sure that she’s wearing a mask so she doesn’t transmit to the baby. The other thing that’s really interesting, is babies don’t seem to get COVID, and when they do it’s usually asymptomatic, without any problems or mild. So we’ve made it — we have all these policies and procedures. Now in the past, we used to separate the mom and the baby. Now our plan is for a mom who’s COVID positive who’s not extremely sick, we’re actually going to allow baby and mom to room together. That’s what the Centers for Disease Control suggest. Moms just have to wear a mask, have to wear gloves and when they breastfeed, they just have to clean everything, their hands, their breasts and so we are now — we’ve moved into the ability now to care for mom and baby together. And it really — the benefits of doing this it allows the moms to breastfeed. The benefits of breastmilk are so huge and we just make it very, very easy for the mom to do this with a low risk of transmission to her baby.
Scott Gilbert – Well, Dr. Kaiser we obviously —
Dr. Jeff Kaiser – Oh, Scott. Scott, sorry. One more thing. So we’ve had a lot of moms who’ve had COVID and not a one of their babies has turned out to be positive. So I think that just shows that all of our policies and procedures have worked really well. Sorry.
Scott Gilbert – No, no. Absolutely. Very reassuring.
Dr. Jeff Kaiser – Yup.
Scott Gilbert – And Dr. Kaiser, I was just going to say we get a lot of very positive if not glowing feedback about your team online, on social media, and on this interview no exception. It looks like Christy’s weighing in noting that she wanted to note how the nurses and therapists involved with her son’s care in April were so helpful and empowering. We are forever thankful, she says.
Dr. Jeff Kaiser – Yup. We’re very lucky at Penn State. We have some of the best nurses and some of the best respiratory therapists that I’ve worked with in my over 20 years of my career. They explain things. They get parents involved early. They encourage parental holding even though it’s scary to hold a small baby. We have some of the smartest respiratory therapists I’ve ever worked with. They just help us do the little tweaking that gives us the very best outcomes and Christy, you’re really lucky that you were with us and had such great nurses and respiratory therapists. If I had my child or now my grandchild, I would be very happy to have our nurses and respiratory therapists take care of them.
Scott Gilbert – And another kind comment here from David who says thank you Dr. Kaiser for your care. This is actually from Valerie in Buffalo. So another kind remark here. I’m curious what it’s like for you because we’ve been talking a lot about the logistics and the planning and the behind the scenes but —
Dr. Jeff Kaiser – Yup.
Scott Gilbert – — really it comes down to caring for babies, caring for little tiny people, and I’m wondering what it’s like for you as a physician when you’ve helped a baby through the woods and it’s been, you know, some ups and downs as I’m sure there are and you’re able to see that baby go home with mom and dad, what is that moment like for you and for your colleagues?
Dr. Jeff Kaiser – Those are — so I’m a worrier. I worry until the minute that they leave on the elevator, and now it’s the parents can worry. I got to tell you, it brings a tear to your eye. Your hair stands up on end, but what is even more exciting is when those parents bring that baby back to the NICU, maybe when they’re one year old, and they walk on their own into the NICU, and maybe they started life 15 weeks early and when we see that and we see the good work and the good outcomes, it — that’s why we do what we do. You know, we do deal with some bad things, but when we see that it is so endearing and it just keeps us going.
Scott Gilbert – Dr. Jeff Kaiser is Chief of Neonatal Perinatal Medicine at Penn State Health Children’s Hospital. He’s been talking with us all about NICU care this hour. Thank you so much, Dr. Kaiser. We appreciate your time.
Dr. Jeff Kaiser – Scott, thanks a lot and I look forward to answering it — any additional questions. Have a good day.
Scott Gilbert – Thank you very much, and before we go I do want to bring up one other comment because it really points to the importance of everyone on the team at Penn State Health Children’s Hospital. We talked about those who provide care at the bedside, but here Michael posts a comment on this Facebook post noting a huge thanks to the environmental health workers who clean and sanitize in preparation for those patients that require a hospital stay. What a great point. You know, there are so many people who are involved and who the moms and dads see, I’m sure, you know, on regular basis and again, thank you Michael for that comment. Thank you, Dr. Kaiser for your time and thanks to all for your comments and for watching Ask Us Anything About NICU Care, from Penn State Health.
Collapse TranscriptMore AUAAs
Read More
If you're having trouble accessing this content, or would like it in another format, please email Penn State Health Marketing & Communications.
