In your corner: Pediatric Complex Care team advocates for children with multiple medical needs
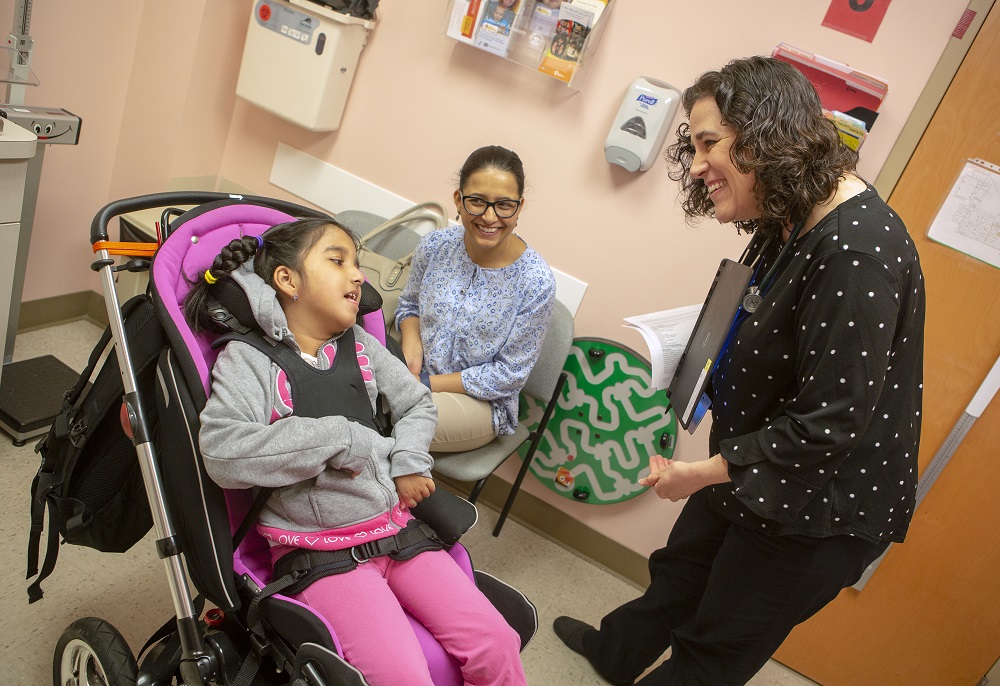
By Carolyn Kimmel
Ask Dina Gonzalez about her son Alejandro’s diagnosis, and she has no specific answer.
The list of health challenges the 10-year-old boy faces, however, numbers at least eight items – seizure disorder, cortical visual impairment, chronic lung disease among them – and managing them is daunting.
“Dealing with the doctors can be hard,” the Lebanon mother said. “A lot of them are good at what they do, but they have tunnel vision for their own specialty, and they don’t take into account all of Alejandro’s conditions and medications.”
Her son uses a wheelchair and requires 24/7 monitoring. Gonzalez says she often feels like a prisoner to his frequent, respiratory-compromising seizures – which require her to give oxygen, stimulation to the chest and rescue breaths.
Worrying about whether insurance will continue to pay for his medical equipment, coordinating all his speech, occupational and physical therapy with specialist appointments and finding time for her older son pose a constant challenge.
Enter Dr. Laura Murphy and the Pediatric Complex Care team at Penn State Health Children’s Hospital.
Since 2009 when she joined the staff, Murphy has made it her personal mission to take on the complicated cases that other doctors shy away from – children who have severely compromised organ systems, are technologically dependent on breathing or feeding tubes, see multiple specialists and require a high degree of coordinated care.

Dr. Shawn Cooper examines the feet of 1-year-old John Peiffer during a checkup.
“These are very medically fragile children who are in and out of the hospital all the time,” said Murphy, who created a similar program at St. Christopher’s Hospital for Children in Philadelphia prior to joining Penn State Pediatrics. “They account for .5% of all children, but they utilize 30% of all health care costs – and most of that is spent in the hospital.”
The number of children requiring complex care is growing as medical interventions have evolved, and they are living longer, she said. The ongoing challenge is how to keep them out of the emergency department and the hospital. A pediatric complex care program is a proven way, Murphy said.
“Families need this kind of care close to home – someone who really knows you,” Murphy said. “We know that hospital readmissions and emergency department visits go down when we are able to manage their care.”
Since Alejandro came under Murphy’s care, his sick admissions to the hospital are down, and he’s only had two seizure-related admissions this year, compared to several times a month previously, his mother said.
The Pediatric Complex Care Team at Penn State Health Children’s Hospital, the only such program in south central Pennsylvania, offers three components:
- A primary care medical home that provides well-child visits, acute visits, after-hours calls and helps families coordinate appointments among specialists, medications, medical equipment, insurance benefits and more. Each child is followed by one of the two complex care physicians and one of the registered nurse clinical case managers, Traci David, Jennifer Coolbeth and Paula Cameron.
- Inpatient consultative service. A member of the team – usually certified physician assistant Samantha Raudensky – rounds with the primary team to see complex care patients daily, providing better continuity between in-patient and outpatient care.
- A presence in the special needs orthopedic and neuromuscular clinics by Dr. Shawn Cooper, who joined the Pediatric Complex Care program last year.
“Dr. Murphy understands Alejandro as a whole, and she cares about how I’m doing too,” Gonzalez said. “She’s eliminated a lot of the fighting I had to do to be heard by his doctors.”
For a weary parent, the value of having a champion to help shepherd care is priceless, she said.
“We are that somebody who is always there for patients and families, who will talk to them day or night in a loving and compassionate way,” Cooper said. “These families need that kind of close relationship.”
Pediatric complex care is often money-losing work for a health system, Murphy said. “There is no doubt that I would be more ‘productive’ seeing healthy kids with minor problems, but this work is greatly needed and highly valuable,” she said – and she is thankful that Penn State Health is making it a priority even though it is not profitable.
The work is demanding and emotionally taxing but extremely gratifying, the doctors say.
“I find more joy than stress,” Cooper said. “I feel more fulfilled personally and professionally when I am helping kids with complicated needs and their families.”
The nature of the patient population means that death is also a regular part of the job.
“We cry with patients, we support each other and then we keep going because there are so many other children who need us,” Murphy said. “At funerals, we see grateful families who pour out to us how we helped them and say they could not have done it without us. It is humbling, to say the least.”
Likewise, Gonzalez is humbled by all the care her family receives. “Even though Dr. Murphy has a million things going on, she takes time for me,” Gonzalez said. And that, in turn, gives her more time for what matters most—her son.

Dr. Laura Murphy talks with Basudha Rizal about her daughter Brinda’s care.
If you're having trouble accessing this content, or would like it in another format, please email Penn State Health Marketing & Communications.
